📖 Deep Dive
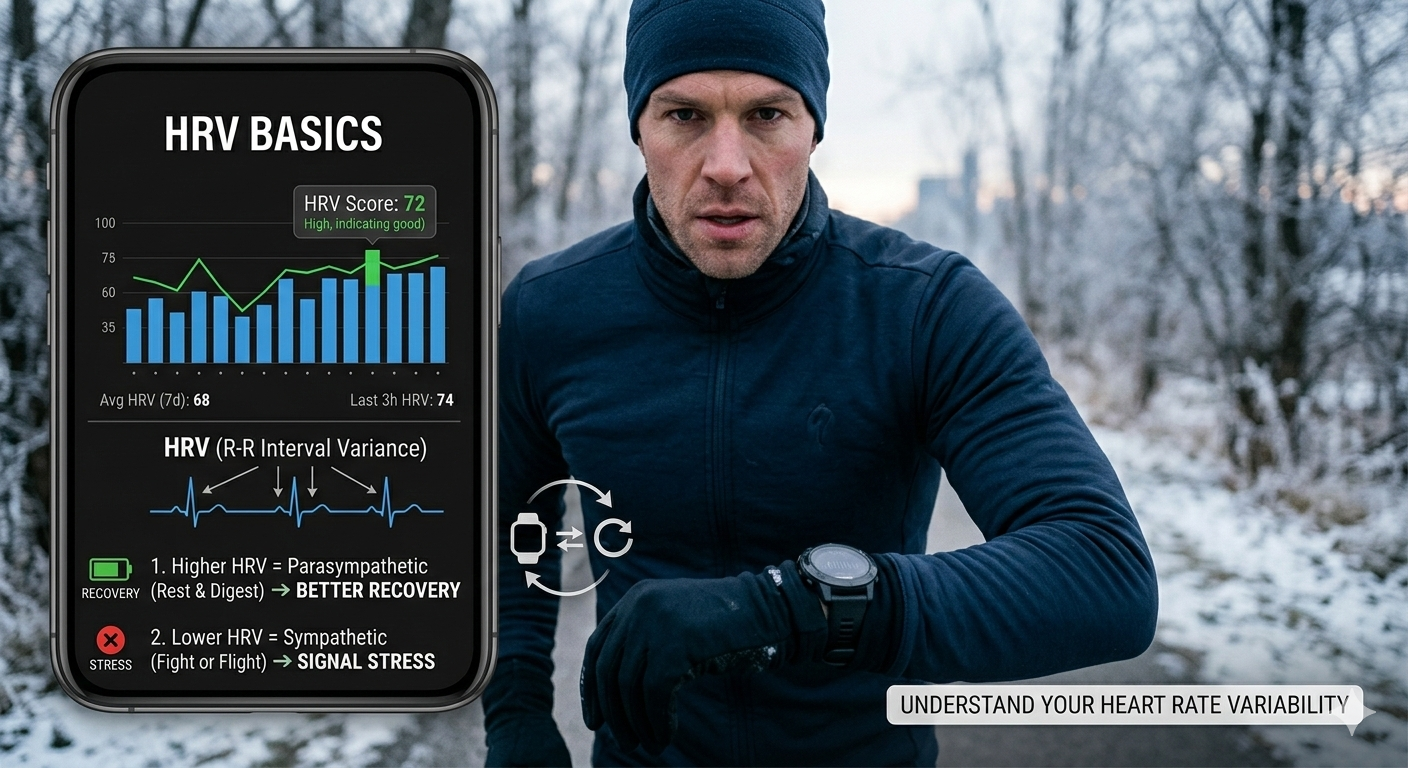
HRV Basics: Understand Your Heart Rate Variability (Any Device)
Heart Rate Variability (HRV) is the beat-to-beat variation in time between heartbeats. Higher, more stable HRV at rest generally reflects a well-recovered autonomic nervous system (strong parasympathetic “vagal” activity), while persistently low HRV suggests accumulated stress, illness, or insufficient recovery. Think of HRV as your body’s real-time recovery telemetry—use it to balance training load, work stress, and sleep so you can progress without burning out.
Quick Metric Reference
| Metric | What it reflects | How devices estimate it | How to use it day-to-day |
|---|---|---|---|
| HRV (RMSSD/SDNN) | Autonomic balance and recovery status | PPG (optical) or ECG; reported as RMSSD (ms), SDNN (ms), or LnRMSSD | Compare to your personal baseline; guide training intensity and recovery |
| Resting HR (RHR) | Cardiac efficiency and acute stress | Lowest nightly or morning HR | Rising RHR with falling HRV indicates strain or illness risk |
| Readiness/Recovery Score | Composite of HRV, sleep, strain | Platform-specific algorithm | Use as a summary; verify with raw HRV trend and how you feel |
| VO2 Max (estimate) | Aerobic capacity | Running pace/HR models; sometimes optical | Long-term fitness trend; not a day-to-day recovery gauge |
How HRV Is Measured (and Why It Differs Across Devices)
- Sensor type
- ECG (chest strap or ring with ECG): very accurate R–R intervals, ideal for short morning spot checks.
- PPG (watch/ring optical): convenient for all-night sampling; sensitive to motion and perfusion.
- Timing
- Overnight: captures long, stable windows during deep sleep; minimizes confounders.
- Morning spot (1–5 minutes): reliable if standardized (same position, breath, time).
- Reported format
- RMSSD (ms): common in recovery apps and rings/wearables.
- SDNN (ms): often used in brief spot readings (e.g., phone/watch apps).
- LnRMSSD: natural-log transform of RMSSD; stabilizes day-to-day variability.
| Approach | Pros | Cons | Typical Use |
|---|---|---|---|
| Overnight PPG (median RMSSD) | Large sample, low effort; good trend detection | Optical artifacts; device algorithms vary | Rings/watches; recovery platforms |
| Morning ECG spot (LnRMSSD) | High signal quality; standardized context | User compliance required; short snapshot | Chest straps; phone-camera apps |
| All-day HRV | Context-rich; detects stress windows | Confounded by movement, posture, caffeine | Stress tracking in smartwatches |
Science in brief: HRV derives from autonomic nervous system modulation of the sinoatrial node. RMSSD captures short-term, high-frequency variability linked to parasympathetic activity; SDNN summarizes overall variability. For endurance and strength training management, RMSSD (or LnRMSSD) is the most-used marker.
Build Your Baseline (The Only Number That Matters)
- Collect 14 days of consistent readings (overnight or standardized morning). Avoid comparing absolute values to others.
- Define baseline: use the 7-day rolling median HRV (RMSSD) and its typical range (e.g., median ± 1 standard deviation or median ± 7%).
- Flag outliers:
- Green: within baseline band or above.
- Amber: 8–20% below baseline or >1 SD down.
- Red: >20% below baseline or >2 SD down.
- Pair with RHR: rising RHR (+3–7 bpm above personal low) alongside a low HRV increases confidence that you’re strained.
Actionable Daily Decisions (Push vs Rest)
| Status | Data Pattern | Decision | Training Prescription |
|---|---|---|---|
| Push | HRV ≥ baseline; RHR near low; feel good | Proceed with planned intensity | Quality session; full volume; limit late caffeine/alcohol |
| Maintain | HRV 3–7% below baseline; RHR stable | Keep session, cap intensity | Reduce intensity 10–20% or shorten intervals; add mobility |
| Deload | HRV 8–20% below; or small drop 2–3 days in a row | Shift to technique/aerobic base | Zone 1–2 only; reduce volume 20–40%; prioritize sleep |
| Recover | HRV >20% below or drop + RHR + symptoms | Rest and monitor | Walk, breathwork; no intensity; hydrate; reassess tomorrow |
Interpreting Your Charts (What to Look For)
- Nightly HRV curve: a smooth, upward trend across the night is typical as parasympathetic tone rises; flat or suppressed curves after alcohol, late meals, or illness.
- 7–30 day trend: look for gradual drifts, not single-day spikes. A steady, week-over-week climb often accompanies effective aerobic blocks; sustained decline signals overreaching or stress spillover.
- Coefficient of Variation (CV): day-to-day swing. High CV (>12–15%) with average HRV falling often means unstable recovery; emphasize consistency (sleep, nutrition).
- Context bands: use a rolling baseline band on your chart; make decisions when values exit this band rather than reacting to any single point.
Common Confounders (Before You Panic)
- Alcohol: even 1–2 drinks can depress HRV and raise RHR for 24–48h.
- Late meals/heavy fat: increases overnight metabolic load; HRV down, RHR up.
- Travel/altitude/heat: acclimation stress lowers HRV temporarily.
- Illness/onset: HRV often drops 1–3 days before symptoms; pair with RHR and subjective feel.
- Measurement posture and breath: for morning spot checks, use the same position (supine or seated), 1:1 relaxed nasal breathing, no talking.
Numbers You’ll See (and How to Translate Them)
| Label on Device | What It Means | Typical Range (Adults) | How to Compare |
|---|---|---|---|
| HRV (ms) | Usually RMSSD in milliseconds | 20–90+ ms (highly individual) | Only vs your own 7–30 day baseline |
| LnRMSSD | Natural log of RMSSD | ~3.0–4.8 (device-dependent) | Track direction and % change, not absolute |
| SDNN (ms) | Overall variability (short + long term) | 30–100+ ms | Useful in standardized short tests |
Formula intuition: RMSSD = sqrt(average of squared differences between successive R–R intervals). It emphasizes fast, beat-to-beat changes driven by parasympathetic activity.
Practical Protocols (Consistency Wins)
- Overnight method: wear your device snugly; aim for 7–9 hours time in bed; avoid alcohol and heavy meals 3–4 hours before sleep; review the nightly median HRV.
- Morning spot method: after waking, bathroom, then 3–5 minutes supine or seated with minimal movement; same time window daily; chest strap or validated app if possible.
- Baseline maintenance: recalc 7-day median weekly; use 30-day view to set season context.
Linking HRV to Training and Life Load
- Endurance blocks: target a rising or stable HRV with small, temporary dips after key sessions; if HRV stays low for >3 days, deload.
- Strength focus: HRV may be less responsive session-to-session; use HRV + RHR + bar speed/RPE to manage fatigue.
- High-stress weeks (work, travel): preemptively reduce intensity 10–20% when HRV trends down, even if training plan says “hard”.
Device/Platform Notes (Objective, General)
- Overnight wearables (rings/watches) often report median RMSSD across the night and a readiness/recovery score. Trust the HRV trend, not the single composite number.
- Smartwatch spot readings may show SDNN over 1 minute. Use a consistent morning reading or rely on nightly auto-tracking if available.
- Chest straps plus apps can provide high-fidelity morning LnRMSSD. Great for athletes needing strict standardization.
Decision Tree: Today’s Call
- Step 1: Is today’s HRV within your 7-day baseline band?
- Yes → Step 2.
- No, down 8–20% → Deload.
- No, down >20% or with symptoms → Recover.
- Step 2: Is RHR within 2 bpm of your low and you feel normal?
- Yes → Push.
- No (RHR +3–7 bpm) → Maintain.
- Step 3: Any confounders last 24–48h (alcohol, late meal, travel)?
- Yes → Discount a single low day; focus on trend.
- No → Follow decision above.
Key Takeaways
- Anchor on your personal baseline, not population averages.
- Pair HRV with RHR and subjective feel to raise decision confidence.
- React to patterns, not points: 2–3 day trends over 1-day blips.
- When HRV is low, reduce intensity/volume and prioritize sleep, hydration, and nutrition.
Note: HRV is a recovery and stress marker, not a diagnosis. If you see persistently depressed values with symptoms, consult a qualified professional.